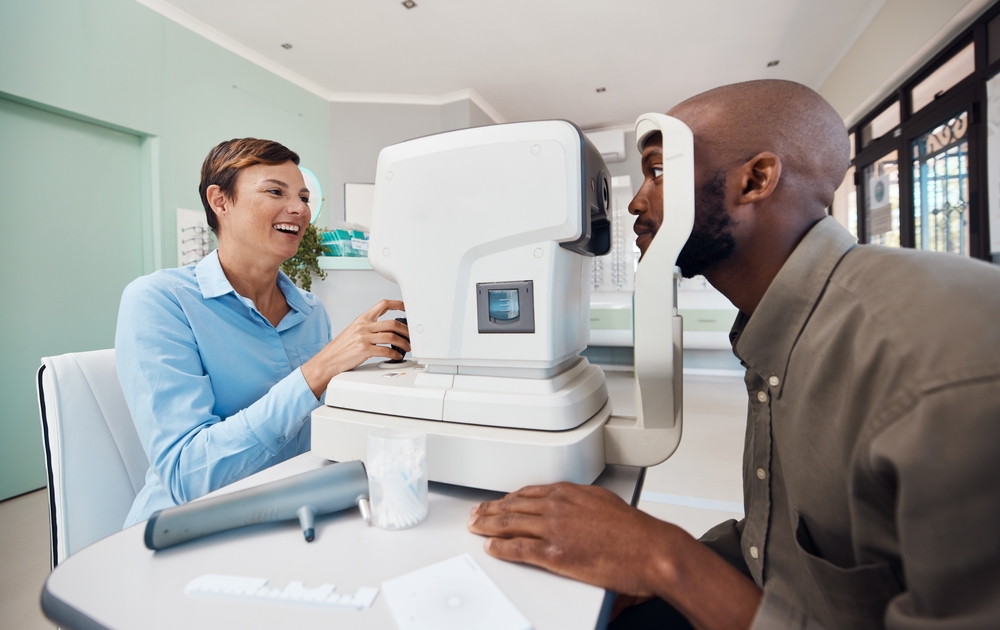
A glaucoma diagnosis changes the way you need to think about your eye health. The condition can progress gradually and without warning, which means the choices you make day to day have more impact than most people expect. Missing appointments, skipping drops, or not knowing which exercises to avoid can all have significant consequences over time.
If you’ve been managing glaucoma for a while, or you were recently diagnosed, knowing what not to do is just as valuable as knowing what to do. Here are six common mistakes that can worsen glaucoma progression, along with practical steps to avoid them.
1. Not Attending Regular Eye Exams

Glaucoma is often called a silent disease for good reason. In its most common form, primary open-angle glaucoma, there are no noticeable symptoms in the early stages.
Vision loss begins at the periphery and moves inward so gradually that many patients don’t realize it until significant damage has already occurred. Regular eye exams are the primary way to catch that damage early and slow it down.
The Glaucoma Research Foundation recommends that adults under 40 be examined every two to four years, with that frequency increasing as you age. Skipping or delaying exams gives glaucoma more room to advance undetected.
There is no substitute for an in-office measurement of your intraocular pressure (IOP) and a thorough evaluation of your optic nerve. Catching changes early is the single most effective way to preserve your vision in the long term.
2. Not Using Your Eye Drops on Schedule
Of all the risk factors associated with glaucoma, elevated intraocular pressure is the biggest contributor to progressive damage. Prescription eye drops are the most common way to lower IOP, and they work, but only when used consistently.
Missing doses allows IOP to rise back toward elevated levels. Over time, those fluctuations create cumulative stress on the optic nerve and the surrounding vasculature.
Even a few missed days each week can significantly reduce the medication’s protective benefit. Many patients stop using their drops because their eyes feel normal, unaware that glaucoma often causes no discomfort at all. The absence of symptoms doesn’t mean the drops aren’t needed.
Building a reliable routine helps. Tying your drops to an existing habit, like brushing your teeth, eating breakfast, or getting ready for bed, gives your brain a consistent cue. The goal is consistency, not perfection, but making your drop schedule a non-negotiable part of your day is one of the most direct ways to protect your vision.
3. Making Poor Dietary Choices
What you eat and drink has a measurable effect on your eye health, and for glaucoma patients, certain dietary patterns can either support or undermine IOP management.

Dark leafy greens are one of the most researched dietary factors in glaucoma. They’re high in dietary nitrates, which the body converts to nitric oxide after ingestion. Nitric oxide supports the drainage of aqueous fluid from the eye and helps maintain healthy blood flow to the optic nerve.
Caffeine is another factor worth paying attention to. A meta-analysis published in recent years found that caffeine consumption was associated with a transient IOP increase in patients with existing glaucoma or ocular hypertension, with IOP rising as much as 2.4 mmHg one hour after intake.
That effect was less pronounced in healthy individuals without glaucoma. If you have a family history of glaucoma or a genetic predisposition, heavy caffeine consumption carries added risk.
Chronic alcohol use also warrants attention. A systematic review of ten studies found that regular alcohol consumption was associated with higher IOP and increased odds of open-angle glaucoma.
4. Exercising the Wrong Way (or Not Exercising at All)
Moderate aerobic exercise is consistently supported in the literature as beneficial for patients with glaucoma. Walking, cycling, and jogging have all been shown to transiently reduce IOP during and after activity.
Research by Lee and colleagues found that for every 5,000 additional daily steps, or approximately 2.5 hours of non-sedentary activity per day, visual field progression was reduced by about 10%. A separate study found that each additional 10 minutes of evening activity was associated with a 15% reduction in the odds of visual field progression in patients with open-angle glaucoma.
That said, not all forms of exercise offer the same benefits. Inverted yoga positions, such as downward-facing dog, forward bends, and headstands, have been shown to significantly increase IOP by placing the eyes below heart level.
Heavy isometric weightlifting exercises can also cause transient IOP spikes, with some leg press movements pushing pressure as high as 41 mmHg during the activity. These spikes may be harmless for most people, but they pose a real risk for patients whose optic nerves are already vulnerable.
5. Smoking
The relationship between smoking and glaucoma is not perfectly linear, but the weight of evidence points in a clear direction. Compounds found in tobacco smoke alter blood flow to the eye, raise the concentration of free radicals, and reduce antioxidant levels in ocular tissue.
Apoptotic and inflammatory markers have been found to be elevated in the aqueous humor of glaucoma patients who smoke, indicating increased cell stress and death. Research has also found that smokers with more than 20 pack-years of history had more than twice the odds of visual field progression compared to non-smokers.
A separate study found that more than eight pack-years of smoking was associated with significantly faster thinning of the retinal nerve fiber layer. These are measurable, structural changes. Quitting smoking removes one of the few controllable factors that accelerate glaucoma damage, and the sooner it happens, the better.
6. Not Wearing Eye Protection

Eye injuries are a preventable cause of glaucoma. Trauma to the eye can disrupt the drainage structures responsible for regulating IOP, leading to what is called traumatic glaucoma or secondary glaucoma. In some cases, this type of damage doesn’t become apparent until months or years after the original injury.
Protective eyewear during high-risk activities is one of the simplest habits to adopt. Power tools, contact sports, yard work, and certain home improvement projects all create conditions where debris or impact could reach the eye.
For patients already managing glaucoma, an additional injury to the drainage system adds a complication that is entirely avoidable. The team at Cheema MD Eye Care encourages patients to keep protective eyewear accessible at home and to wear it consistently whenever necessary.
Protecting Your Vision Is an Ongoing Effort
Managing glaucoma progression well requires more than just showing up to appointments and filling prescriptions. The everyday habits outlined here, staying consistent with drops, eating a balanced diet, choosing the right exercises, avoiding tobacco, and protecting your eyes from injury, all reinforce each other. None of them alone will stop glaucoma, but together they give your treatment plan its best chance of working.
If you have questions about your current glaucoma management plan or want a comprehensive evaluation, schedule an appointment at Cheema MD Eye Care in Kingston, NY, today. Our team is here to help you stay proactive about your long-term vision.